 Cleanzine: your weekly cleaning and hygiene industry newsletter 21st May 2026 Issue no. 1211
Cleanzine: your weekly cleaning and hygiene industry newsletter 21st May 2026 Issue no. 1211
Your industry news - first
The original and best - for over 20 years!
We strongly recommend viewing Cleanzine full size in your web browser. Click our masthead above to visit our website version.
Hand hygiene in the NHS: Parliament debates
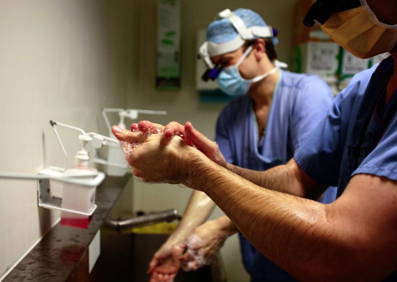 A debate was scheduled to take place in Westminster Hall on the motion: 'This House has considered hand hygiene in the NHS'. The debate was tabled by Nigel Mills MP, who has a keen interest in healthcare and hygiene issues.
A debate was scheduled to take place in Westminster Hall on the motion: 'This House has considered hand hygiene in the NHS'. The debate was tabled by Nigel Mills MP, who has a keen interest in healthcare and hygiene issues.
"I tabled this debate to request that the Government ensure that proper checks are introduced so that patients can have confidence that everything possible is being done to enforce proper hand hygiene best practice," he said earlier this week.
"At a time when we are experiencing rising levels of antimicrobial resistance, we need to concentrate on how we can prevent infections in the first place.
"Healthcare Associated Infections represent a worrying trend across the healthcare profession. According to 2011 data, patients in England have a 6.4% chance of contracting an HAI - if people visiting a restaurant had a 6.4% chance of contracting an infection, that restaurant would not be able to continue to operate, so why are we tolerating such levels of HAIs in our hospitals?
"Here in the UK, HAIs affect more than 300,000 patients every year, resulting in 5,000 deaths and costing UK hospitals up to £1billion every year. It's thought that more than 30% of HAIs could be avoided simply through better application of existing knowledge and realistic infection control practices - which would save lives and prevent unnecessary and prolonged hospital stays.
"Currently, in the NHS, under National Institute for Health & Care Excellence guidelines, best practice is measured using 'direct observation', with nurses manually counting the number of handwashes versus opportunity.
"The problem is that people tend to change their behaviour when they are aware that they are being observed - known as the 'Hawthorne Effect' - which is thought to artificially increase compliance rates by over 50%.
"Moreover, under the current guidelines, trusts are simply required to audit hand hygiene practices and capture the data locally; no onward reporting, review or validation of this vital data is required or in place.
"UK trials using 24/7 electronic monitoring demonstrate that hand hygiene compliance rates are actually in the region of 18% - 40%, as opposed to the 90% -100% reported by hospital wards. The current methods of reporting are not only inaccurate, they're also taking up valuable nursing time which could be applied elsewhere if more accurate reporting methods were employed.
"I would like to see every NHS trust introduce a hygiene improvement programme, as current methods for auditing hand hygiene compliance are outdated and data is hugely overstated. Sir Mike Richards, chief inspector of hospitals for the Care Quality Commission, has highlighted the inaccuracy of local hand hygiene audits.
"I am therefore asking the Government and the Department for Health to make sure Care Quality Commission and hospital trusts introduce proper checks on hand washing. The incidence of HAIs highlight that current checks are woefully inadequate - as, whilst hospitals are reporting higher levels of compliance, this isn't supported by the rates of HAIs. I would like to see the Government introduce measures to reduce the rate of HAIs and look closely at how data is collected to ensure data on hand hygiene is captured accurately to ensure quality improvements.
"This is a priority patient safety issue and I am working closely alongside Andrea Jenkyns MP, who recently launched the Handz campaign (www.handz.org.uk), to raise awareness on the importance of hand hygiene."
According to NICE, around one in 16 people being treated on the NHS in England each year picks up an infection. As a result, more NHS resources are consumed and the affected patients are at increased risk.
Effective hand decontamination, even after wearing gloves, results in significant reductions in the carriage of potential pathogens on the hands and decreases the incidence of preventable healthcare-associated infections, leading in turn to a reduction in morbidity and mortality. Hand decontamination is considered to have a high impact on outcomes that are important to patients. Although hand hygiene has improved over recent years, remaining misconceptions about this standard principle of infection control are reported and good practice is still not universal.
Since Quarter 2 of 2012 there has been a 27% decrease in the rate of total MRSA bacteraemia reports when compared to the latest Quarter for which results have been analysed (Quarter 3 2015) - down from 1.1 to 0.8 reports per 100,000 bed days. This is part of an overall decreasing trend beginning April 2007. However, the rates of Trust assigned MRSA bacteraemia reports in Quarter 3 2015 have increased by 14.0% (when compared to the same quarter in the previous year (0.7 to 0.8 per 100,000 bed-days).
MSSA (Methicillin-sensitive Staphylococcus aureus) rates have also increased when comparing Quarter 3 of 2015 with Quarter 3 of 2014 - up to 8.2 per 100,000 bed days from 7.9.
C.Difficile rates for Quarter 3 of 2015 were the same as in the third quarter of 2014, however rates have fallen since 2012.
According to the latest World Health Organisation figures, released in May 2014 following a global survey, of every 100 hospitalised patients, at least seven in high-income and 10 in low- /middle-income countries will acquire a healthcare-associated infection. Among critically ill and vulnerable patients in intensive care units, that figure rises to around 30 per 100.
The results of the global survey confirmed that resistance is very frequent in bacteria isolated in healthcare facilities; for instance, for MRSA, it is as high as 44%, 40% and 38% on average in Latin America, West African countries, and Europe respectively.
www.parliament.uk / www.politicshome.com / www.twitter.com
14th January 2016







