 Cleanzine: your weekly cleaning and hygiene industry newsletter 28th May 2026 Issue no. 1212
Cleanzine: your weekly cleaning and hygiene industry newsletter 28th May 2026 Issue no. 1212
Your industry news - first
The original and best - for over 20 years!
We strongly recommend viewing Cleanzine full size in your web browser. Click our masthead above to visit our website version.
Healthcare settings see spread of new drug-resistant fungal infection
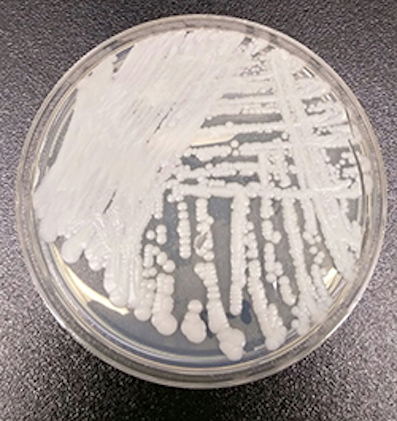 Thirteen cases of Candida auris - a serious and sometimes fatal fungal infection that is emerging globally, with cases documented in Japan, South Korea, South Africa, Kuwait, India, Pakistan, Venezuela, Colombia and the UK - have now been identified in the US, according to the Centers for Disease Control and Prevention.
Thirteen cases of Candida auris - a serious and sometimes fatal fungal infection that is emerging globally, with cases documented in Japan, South Korea, South Africa, Kuwait, India, Pakistan, Venezuela, Colombia and the UK - have now been identified in the US, according to the Centers for Disease Control and Prevention.
C. auris is often resistant to antifungal drugs and tends to occur in hospitalised patients.
In June 2016, CDC issued a clinical alert describing its global emergence and requesting that laboratories report C. auris cases and send patient samples to state and local health departments and CDC, to monitor the infection's spread and ensure that effective infection control procedures are followed to limit its spread.
"We need to act now to better understand, contain and stop the spread of this drug-resistant fungus," says CDC director Tom Frieden, M.D., M.P.H. "This is an emerging threat, and we need to protect vulnerable patients and others."
Among the seven cases detailed in the report, patients with C. auris were reported in four states: New York, Illinois, Maryland and New Jersey. All of the patients had serious underlying medical conditions and had been hospitalised an average of 18 days when C. auris was identified. Four of the patients died; it is unclear whether the deaths were associated with C. auris infection or underlying health conditions.
In two instances, two patients had been treated in the same hospital or long-term-care facility and had nearly identical fungal strains. These findings suggest that C. auris could be spread in healthcare settings.
Six of the seven cases were identified through retrospective review of hospital and reference laboratory records. Identifying C. auris requires specialised laboratory methods because it can easily be misidentified as another type of Candida infection, in which case patients may not receive appropriate treatment. Most of the patient samples in the current report were initially misidentified as another species of Candida.
Most of the C. auris strains from US patients (71%) showed some drug resistance, making treatment more difficult. Samples of strains from other countries have been found to be resistant to all three major classes of antifungal medications. However, none of the US strains in this report were resistant to all three antifungal drug classes. Based on laboratory testing, the US strains were found to be related to strains from South Asia and South America. However, none of the patients travelled to or had any direct links to those regions. Most patients likely acquired the infections locally.
Tom Chiller, M.D., M.P.H., chief of CDC's Mycotic Diseases Branch, says: "It appears that C. auris arrived in the United States only in the past few years.
"We're working hard with partners to better understand this fungus and how it spreads so we can improve infection control recommendations and help protect people."
CDC recommends that healthcare professionals implement strict Standard and Contact Precautions to control the spread of C. auris. Facilities should conduct thorough daily and after-discharge cleaning of rooms of C. auris patients with an EPA-registered disinfectant active against fungi. Any cases of C. auris should be reported to CDC and state and local health departments. CDC can assist in identifying this particular type of Candida if needed.
In 2013, CDC issued a report describing antibiotic resistance threats in the US that needed prompt action, including Candida infections. CDC's Antibiotic Resistance Laboratory Network is providing additional lab support in four regional laboratories to test fungal susceptibility of Candida species and identify emerging resistance. CDC is also expanding tracking of this fungus through the Emerging Infections Program. Information gathered through these networks plays a key role in tracking resistance and informing policies and interventions.
The challenge of emerging antibiotic resistant threats like C. auris highlights the need for urgent, coordinated, international public health response and the importance of CDC's AR Solutions Initiative. The timely investments in the AR Solutions Initiative empower CDC to rapidly detect, investigate, and respond to emerging threats, like C. auris; prevent resistant infections from occurring and spreading across healthcare settings and the community; and innovate, supporting development of new diagnostics and drugs to test, treat, prevent infections, and save lives.
Sporadic cases of C. auris have been identified throughout England since August 2013, with a total of 12 isolates among eight patients sent to the Public Health England Reference Mycology Laboratory. Since April 2015, an adult critical care unit in England has been managing an outbreak of C. auris, with more than 40 patients either colonised or infected; approximately 20% with candidaemia. The hospital outbreak has been difficult to control, despite enhanced infection control interventions, including regular patient screening, environmental decontamination and ward closure. In addition, two further positive isolates have been identified at the PHE Reference Mycology Laboratory in 2016 which were submitted from another hospital in a different region; investigations are ongoing to identify if there are any further cases. Of note, one of these isolates is phenotypically distinct to the outbreak strain.
In June 2016, PHE alerted healthcare providers, including microbiologists and infection prevention and control personnel, to the emergence of this fungal pathogen. In addition, guidance was published for the laboratory investigation, management and infection prevention and control of cases of Candida auris.
10th November 2016







